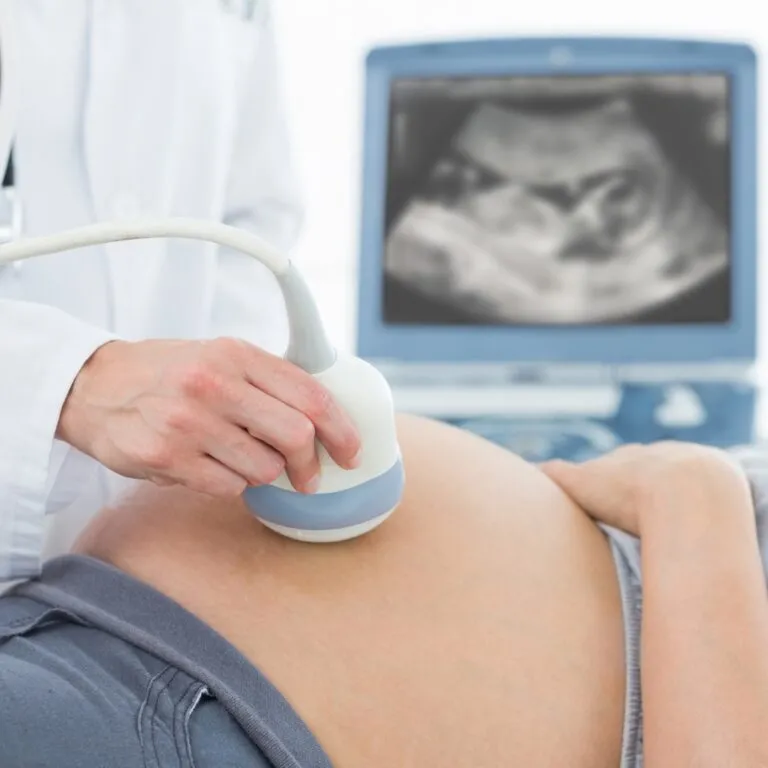
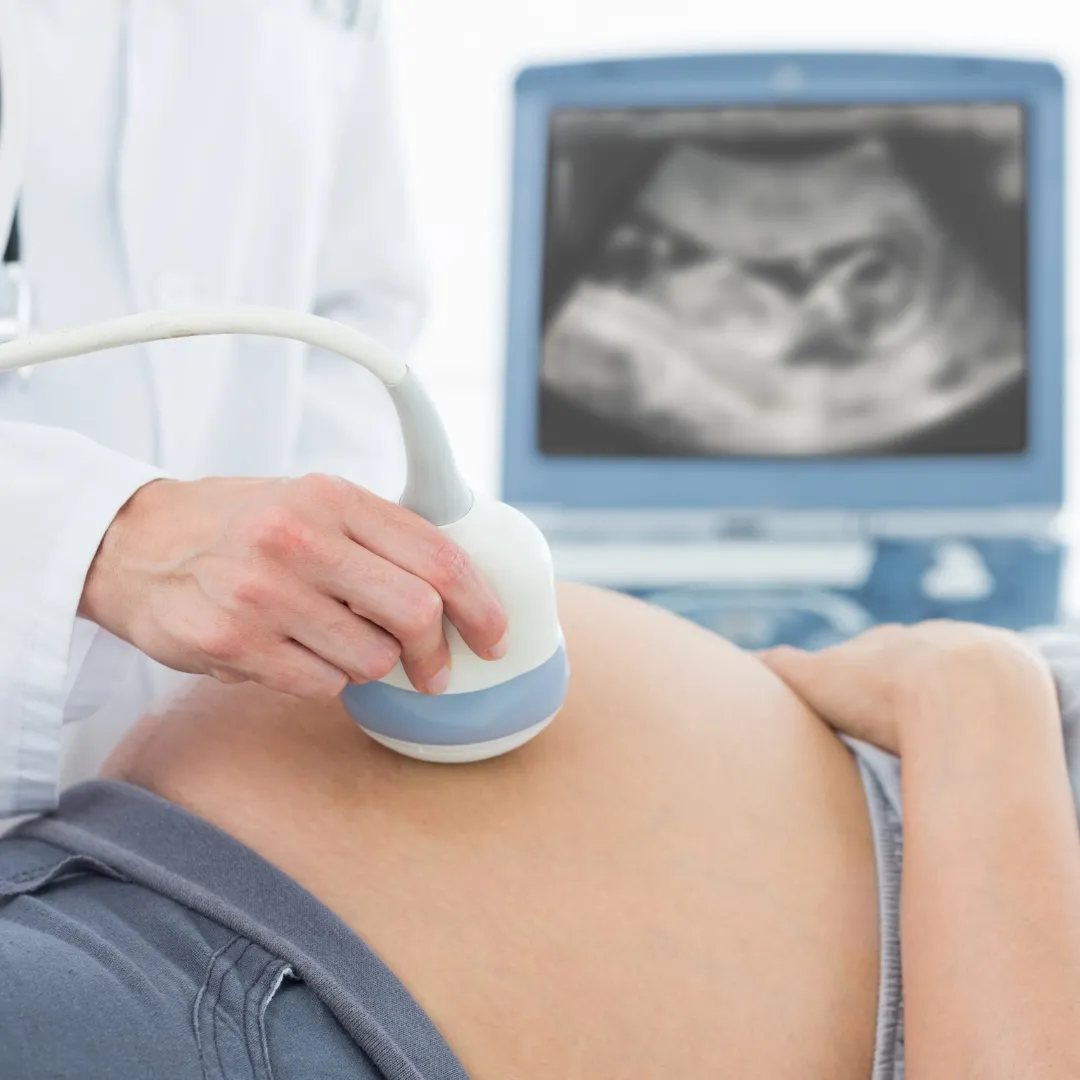
“What to expect when you’re expecting” is a phrase that doesn’t just refer to the growing bump, influx of hormones and other symptoms, but to everything else that comes along with it, including the midwife appointments and tests and screenings.
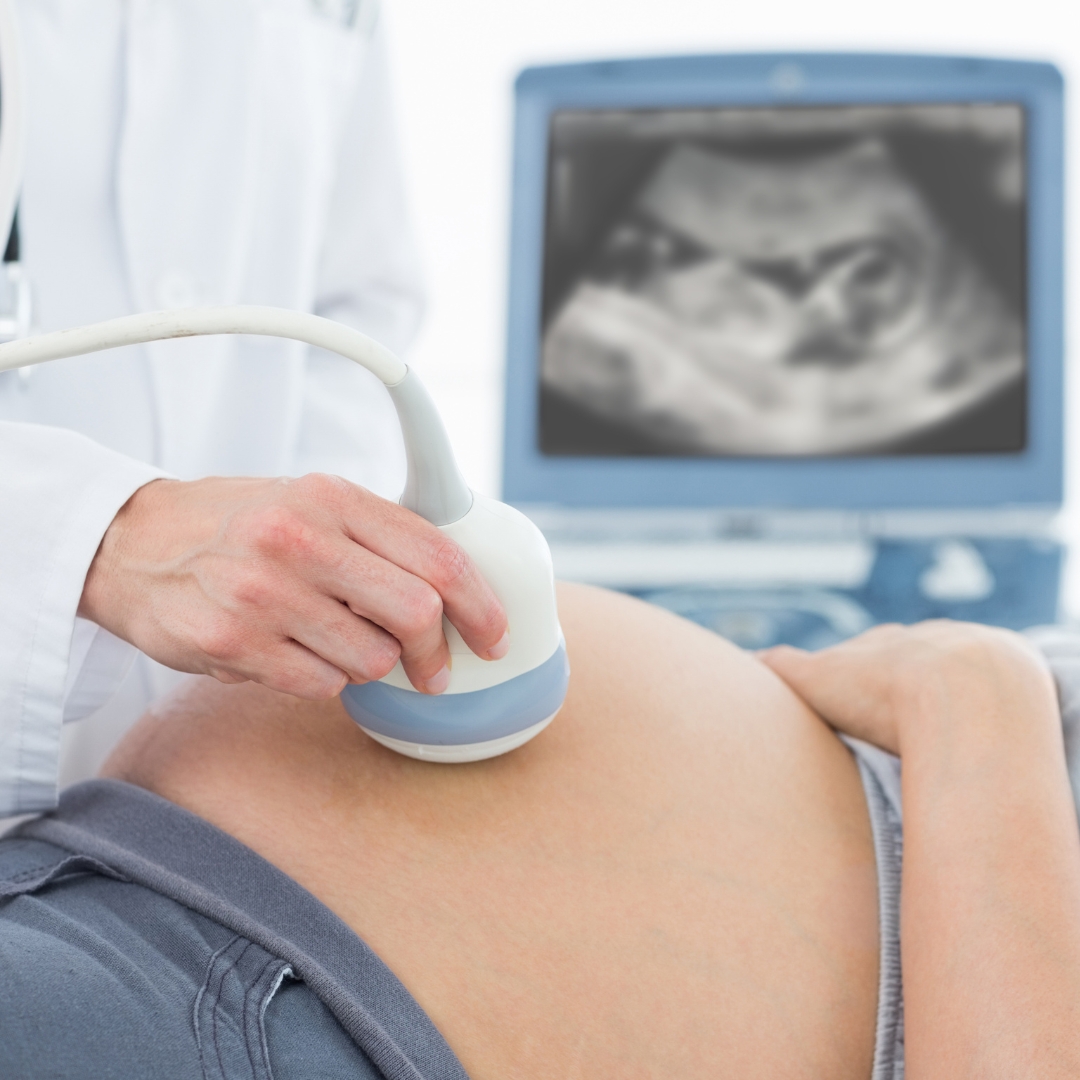
Congratulations! Whether you’ve just seen that first positive result on a pregnancy test or you are navigating the exciting middle weeks, your journey is punctuated by a series of vital milestones. In the UK, prenatal care is designed to monitor the health of both you and your unborn baby, providing a safety net of medical care through routine and specialized diagnostic testing.
“What to expect when you’re expecting” is a phrase that doesn’t just refer to the growing bump, influx of hormones and other symptoms, but to everything else that comes along with it, including the midwife appointments and tests and screenings.
[Post updated March 2026]
Understanding the difference between a screening test result (which assesses risk) and a diagnostic procedure (which provides a definitive answer) is key to navigating your prenatal visits with confidence. This guide breaks down every ultrasound exam, blood sample, and urine test you’ll encounter, alongside how these moments align with future-proofing your baby’s health through Smart Cells stem cell banking.
First Trimester: Building the Foundation (Weeks 1–12)
The first trimester of pregnancy is a whirlwind of biological changes. During these early pregnancy weeks, your healthcare provider focuses on establishing a baseline for your health and screening for genetic conditions.
If you’d like to know more about what’s going on in your body and with your baby in the first trimester of pregnancy, we have a useful guide here.
The Booking Appointment (Weeks 8–10)
Your first official date with a health professional (usually a midwife) is the booking appointment. This is more than just paperwork and chatting. You’ll go over a comprehensive review of risk factors and family history.
This initial meeting is crucial for identifying if you require more specialised maternal care or if you might be categorised as having a high-risk pregnancy due to pre-existing health conditions. It’s also a great way to meet your community midwifery team and start to build your relationship with them. If you’d like to know more about what midwives are and what they do, we have a whole post about what midwives do here.
At this first appointment with a midwife, you can expect them to:
- Check your blood pressure, height, and weight.
- Test your urine for protein or signs of infection.
- Arrange for blood tests to check your blood group, iron levels, and immunity to certain infections.
The blood tests may be used for the following:
- Blood Sample & Blood Type: You’ll have a simple blood test to determine your blood type and Rh factor. If you are Rhesus negative, your pregnancy care provider will discuss the need for Anti-D injections to prevent complications.
- Infectious Disease Screening: These tests check for HIV, Hepatitis B, and Syphilis. Early detection allows for medical care that significantly reduces the risk of transmission to your baby.
- Carrier Screening: Depending on your background, you may be offered screening for sickle cell disease, thalassaemia, or cystic fibrosis.
The Dating Scan (Weeks 10–14)
This is often the first time you’ll see your baby! Using sound waves via an abdominal ultrasound (or occasionally a transvaginal ultrasound if the baby is tucked away or it turns out that you’re earlier in your pregnancy than expected), the sonographer confirms:
- The number of weeks gestation to confirm your due date (which, as we all know, is an estimation – find out more about due dates here)
- The heart rate.
- Whether you are expecting one baby or multiples – if you get a surprise about twins, triplets or more here, read more about cord blood banking for multiples here.
First Trimester Screening (The Combined Test)
Conducted between 10 and 14 weeks of pregnancy, this combines a maternal blood test with something called a nuchal translucency scan. This screening test result calculates the likelihood of chromosomal disorders such as down syndrome (Trisomy 21), Edwards’ syndrome, and Patau’s syndrome. This often happens around the same time as, or is combined with, the dating scan. It is designed to estimate your baby’s risk of these conditions, alongside certain factors like measurements.
This is the perfect time to start researching stem cell banking. As you learn about your baby’s genetic makeup, consider how storing umbilical cord blood can provide a biological insurance policy against over 80 health conditions later in life.
Second Trimester: Detailed Development (Weeks 13–27)
In the second trimester, the focus shifts from “is the pregnancy viable?” to “is the baby developing correctly?” Many parents look forward to the scan that comes in the second trimester as it’s a chance to see your little one in much more detail, and you can sometimes even tell the sex of the baby!
The Anomaly Scan (Weeks 18–21)
This detailed ultrasound scans the baby from head to toe. The sonographer looks at the structure of the heart, brain, spine, and kidneys to identify physical problems or birth defects such as spina bifida or neural tube defects.
During this scan, the healthcare provider will also check the position of the placenta to ensure it isn’t blocking the cervix, a condition known as placenta previa, and will check for any other complications with the placenta which could impact your birth plan.
Glucose Screening & Gestational Diabetes
Around weeks 24–28, you may be offered a glucose challenge test or a more detailed glucose screening (OGTT) if you have risk factors for gestational diabetes. This condition causes high blood sugar that can affect your baby’s growth and lead to pregnancy complications. You will have two blood tests on either side of having a sugary glucose drink to measure how your body processes sugar. Managing gestational diabetes is vital, as untreated high blood sugar can lead to a larger baby (macrosomia), making delivery more complex or leading to complications for the mother during pregnancy and labour.
Third Trimester: Preparing for Birth (Weeks 28–40)
The third trimester is about monitoring baby’s growth and ensuring your body is ready for the marathon of labour!
Routine Monitoring
At every appointment, you will provide a urine sample to check for protein which is a key indicator of high blood pressure or pre-eclampsia. You will also have your fundal height measured. This is when your midwife uses a tape measure to record the distance between your pubic bone and the top of your uterus. This can help to check that the baby is still measuring on the same growth curve as well as to monitor the baby’s position and amniotic fluid.
Group B Streptococcus (GBS)
While not always routine on the NHS, many pregnant women choose to have a private test for group B streptococcus around week 36. If the test results are positive, antibiotics during labour can protect the baby from serious infection.
Growth Scans
For high-risk pregnancies, your health care provider may request a doppler ultrasound to check the blood flow in the placenta or a biophysical profile to assess the baby’s muscle tone and amniotic fluid levels. You may also be offered a growth scan if, as a result of your fundal height measurement, your midwife suspects that your baby is ahead or behind their growth curve. Most of the time, these scans are simply a reassurance and you’ll need nothing further.
Understanding “High Risk” and Further Testing
If a screening returns an abnormal result or an increased risk, it does not mean your baby has a condition. It simply means additional testing is needed.
Many parents find this stage particularly stressful and have many worries about what this means for their family, but it is important to remember that most screenings that result in higher risk are followed by diagnostic tests that show the baby is perfectly healthy. Your healthcare provider or midwife will be able to discuss options with your for if further testing comes back with results that you weren’t expecting.
| Test | Type | Description |
| NIPT | Screening | Non-invasive prenatal testing analyzes fetal DNA in your blood. It is highly accurate with a low false positive rate. |
| CVS | Diagnostic | Chorionic villus sampling takes a tiny tissue sample from the placenta (usually weeks 11–14). |
| Amniocentesis | Diagnostic | A needle is used to take a sample of amniotic fluid (usually after week 15). |
These diagnostic tests carry a small risk of miscarriage, so you will likely meet with a genetic counselor to discuss the test results and what they mean for your family.
Protecting the Future: Stem Cell Banking
All these prenatal screenings and ultrasound scans are designed to give your baby the best start in life. Stem cell banking with Smart Cells is the logical next step in that protection plan.
Why Store Stem Cells?
The umbilical cord is a rich source of powerful stem cells that can treat genetic disorders, sickle cell disease, and certain cancers. While prenatal tests identify current health problems, private stem cell storage prepares you for future ones.
- Non-invasive: Collection happens after birth and doesn’t interfere with your birth plan.
- Genetic Match: The cells are a perfect match for your baby and a potential match for siblings.
- Emerging Therapies: Research is ongoing for conditions such as cerebral palsy, and even Type 1 diabetes. By choosing to store these cells at a private health center like Smart Cells, you are securing a resource that could be used for life-saving medical care in the decades to come.
FAQs for Expectant Parents
What is the difference between a screening and a diagnostic test?
A screening test result tells you the probability (e.g., 1 in 500) of a condition. A diagnostic procedure like amniocentesis gives a definitive “yes” or “no” but involves more invasive techniques.
What if I get a negative result?
A negative result on a screening means your baby is at higher risk than the general population, but it is not a guarantee of a health problem. Conversely, a low-risk result doesn’t rule out all possibilities.
When should I book my Smart Cells kit?
We recommend finalizing your plan by the start of your third trimester. This ensures your collection kit is ready and your healthcare provider is briefed on the procedure before the big day.
Are ultrasound scans safe for my baby?
Yes, ultrasound exams use sound waves rather than radiation to create images. They have been used in prenatal care for decades with no known side effects for the mother or the unborn baby.
Can I have extra scans if I’m worried?
In the UK, the NHS typically offers two scans. However, many pregnant patients choose to have private pregnancy ultrasounds, such as 4D scans or early reassurance scans, for extra peace of mind, to see the baby’s growth in more detail or to find out the sex of their baby.
What happens if my baby is in the wrong position during a scan?
It is very common for a baby to be curled up or facing the wrong way during an ultrasound exam. If the sonographer cannot get the necessary measurements for the anomaly scan or dating scan, you may be asked to go for a short walk or drink some cold water. If they still can’t see what they need, you will usually be booked in for a follow-up appointment.
Navigating the landscape of pregnancy care can feel overwhelming, but each ultrasound exam and blood test is a tool for clarity. By staying informed and working closely with your health center and health professionals, you can enjoy your pregnancy with peace of mind.

Rate this article: