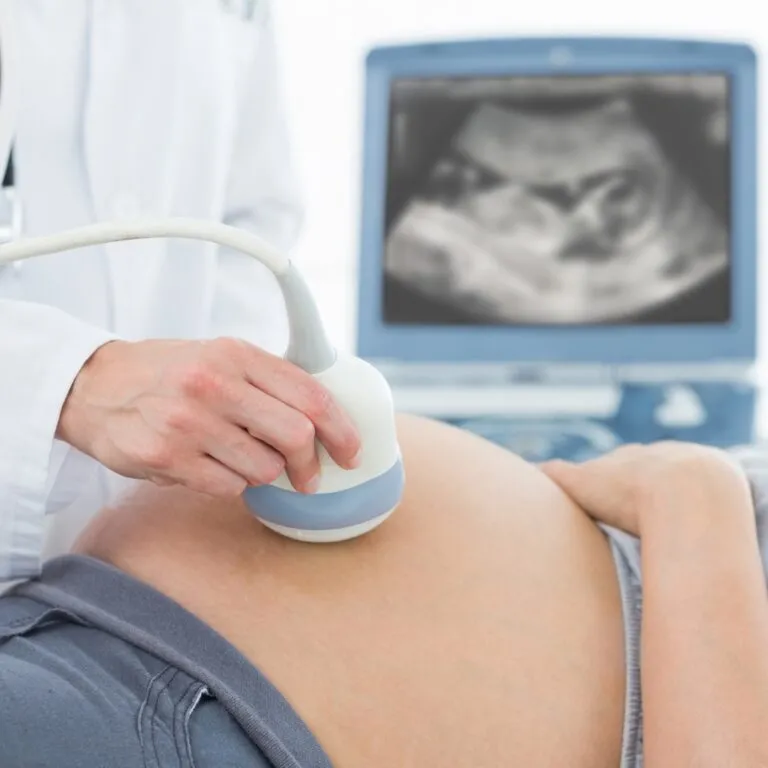
In this article we hear from three sets of parents who have experienced the incredible benefits of stem cell therapy first hand.
The landscape of modern medicine is shifting. While traditional treatments focus on managing symptoms, the field of regenerative medicine is looking toward the source of the problem: damaged cells and tissues. At the forefront of this revolution is stem cell therapy, a treatment modality that is transforming medicine and with it the lives of increasing numbers of patients with life-threatening illnesses.
In this article, we hear from three sets of parents who have experienced the incredible benefits of stem cell therapy first hand. Their stories serve as a powerful proof of concept for the potential of umbilical cord blood and tissue to provide a lifelong safety net.
[Article updated March 2026]

The Science Behind the Success: What Are Stem Cells?
To understand how these stories were possible, we must first look at the biology. Stem cells are the building blocks of the blood and immune system and they have incredible capabilities. They are undifferentiated cells, meaning they have not yet grown into a specific type of cell, such as a heart, muscle, or nerve cell. Because they can develop into different cell types, they offer a versatile foundation for the next generation of cancer treatment and tissue repair.
They can heal and repair cells and tissue, help rebuild the blood and immune system and even transform themselves into other types of cells in order to replace damaged cells. One of the richest sources of stem cells is umbilical cord blood, taken at birth and stored in special blood banks. The procedure is very simple and does not affect mother or baby at all, yet the long-term benefits of storing a newborn’s cord blood could be nothing short of life-saving.
It is now more than 37 years since the first successful cord blood stem cell transplant took place and in that relatively short space of time, this groundbreaking form of medicine has contributed to the successful treatment of more than 80 different diseases, including cerebral palsy, leukemia and sickle cell disease. Through ongoing stem cell research, the list of treatable medical conditions looks certain to rise as researchers report promising results in tests on type 1 diabetes, stroke, multiple sclerosis, autism, Crohn’s disease and other types of cancer.
The three patients in our stories have had their lives transformed by stem cell therapy. Each one has been able to overcome illness thanks to a transfusion of the cord blood stem cells their parents banked for them when they were babies.
Sasha’s Story: A Breakthrough for Cerebral Palsy
When Sasha Browne was born, her parents, Tania and Richard, took the decision to collect and store their new daughter’s umbilical cord blood as an ‘insurance policy’ to safeguard her health for the future. Little did they realise how crucial a step this would prove to be. Sasha was born with cerebral palsy, an umbrella term for a range of different conditions that affect the brain, causing problems with movement, posture and co-ordination.
Cerebral palsy often results from a brain injury or abnormal development that occurs while a child’s brain is still developing, before, during, or immediately after birth. For years, the medical consensus was that brain tissue, once damaged, could not be repaired. However, the emergence of stem cell technology has challenged this “permanent damage” theory. Even today, the research into cerebral palsy stem treatments is still evolving with very promising results.
The Road to Duke University
The family, who are originally from the UK but now live in Dubai, where Sasha was born, agreed for Sasha to go to the US to take part in the first ever stem cell therapy trial to treat cerebral palsy. The trial was led by Dr Joanne Kurtzberg at Duke University, North Carolina, an internationally renowned expert in pediatric hematology/oncology, pediatric blood and marrow transplantation, umbilical cord blood banking/transplantation, as well as the emerging fields of cellular therapies and regenerative medicine.
Three-year-old Sasha is thought to be the first British child to be infused with her own umbilical cord blood stem cells and her parents believe this pioneering procedure has transformed her life, helping to improve her ability to walk, see and speak.
How the Therapy Works
By injecting Sasha with stem cells harvested from her umbilical cord at birth, doctors put healthy stem cells into her bloodstream in the hope that they would help to repair some of the damaged tissue. In cases of neurological disorders, the theory is that these cells can release growth factors and anti-inflammatory cytokines that cross the blood-brain barrier. This process helps to reduce inflammation in the brain and stimulate the body’s own repair mechanisms, a concept known as “paracrine signaling.”
The results for Sasha were very positive.
“We feel there has been some general progress in her motor skills and perhaps some improvement in her vision and cognitive ability,” says Tania. “Sasha’s therapists definitely noticed a change. They would say, “Look at the difference in her – her walking is streets ahead of what it was before. Look at her hand – last time I saw her hand it was really closed and now it’s moving more.””
“We can’t categorically say this is attributable to the stem cell infusion Sasha received; however, both myself and my husband, together with Sasha’s therapist, feel the improvement has potentially been at a faster rate than it may have occurred, or in comparison with other children with similar abilities.”
Sasha does receive other treatments to help with her condition, such as physiotherapy, occupational therapy and hydrotherapy. However, her all-round progress has been so great that a planned operation to correct a squint has now been postponed and may no longer be necessary at all.
Dr Kurtzberg observed improvements in many of the children who took part in the same trial and has gone on to carry out a second phase to establish whether these advances were due to the stem cells or some other placebo effect. Recent studies have continued to build on this, showing that hematopoietic stem cells found in cord blood are a powerful tool for neurological repair and represent an increasingly effective treatment for brain injuries.
Ahmed’s Story: The Power of Sibling Donation
While Sasha used her own cells (an autologous transplant), Ahmed’s story demonstrates why stem cell transplants are often a family-wide resource.
When Mohammed Ahmed and his wife found out they were expecting their second child, they decided they would collect and bank their soon-to-be-born daughter’s precious stem cells in an attempt to help treat their older son, Ahmed, who suffered with thalassemia major. This is an inherited blood disorder, whereby the body is unable to produce hemoglobin, the oxygen-carrying red blood cells, and results in severe anaemia, fatigue and the inability to thrive. In its most severe form it can lead to organ failure and death.
Thalassemia major is a chronic disease that typically requires lifelong blood transfusions and chelation therapy to remove excess iron from the blood. It is a grueling treatment plan that impacts the quality of life for the entire family. For Ahmed, a stem cell transplant offered the only potential for a permanent cure.
A Perfect Match
When new baby Alanoud was born, the stem cells were collected from her umbilical cord and arrangements were put in place for the stem cell transplant for Ahmed to be carried out. Because siblings have a high chance of being a genetic match, Alanoud’s cells were compatible with Ahmed’s body, reducing the risk of immune responses like Graft-versus-Host Disease.
The procedure was a great success and, over a period of six months, Ahmed made a full recovery.
“Ahmed is now seven years old and he is growing in height,” says his father. “He’s now free from transfusions and medication, is going to school and loves playing with the other kids and simply enjoys being just like the other kids. I would definitely say parents who have children diagnosed with thalassemia should not delay in getting stem cell therapy for their children because the longer you wait, the greater their health can deteriorate.”
“Without having stored the stem cells of his newborn sister, my son would not have recovered from his illness. Everyone should know about the potential of stem cell therapy and how it can save lives. I will have no hesitation in collecting and storing the cord blood stem cells when our next baby is born.”
Hematopoietic Stem Cells and Blood Disorders
Ahmed’s recovery was made possible by hematopoietic stem cells. These are specific cell types that have the ability to “reboot” the patient’s immune system and blood production. Once infused, these cells travel to the bone marrow, where they begin producing healthy red blood cells that contain the proper hemoglobin, effectively ending the need for external transfusions. This same biological mechanism makes these cells the standard of care for various blood cancers and other bone marrow failures.
Paige’s Story: An Investment in Future Safety
When their first child was due in December 2012, Kyle and Carla Poppleton, who live in Botswana, made the decision to arrange for the collection and storage of their new baby’s cord blood and tissue stem cells. The couple had thoroughly researched the topic and realised that the opportunity to take advantage of this pioneering form of medicine and safeguard the health of their new child was an opportunity too important to miss.
Their daughter Paige was born in London in March 2013 but, just under a year later, was diagnosed with mild cerebral palsy. At six months old she could not sit and spent most of the time with her little right hand in a fist and her toes curled up. The Poppletons immediately started an intense course of physiotherapy and occupational therapy for Paige to try to ease the situation. They also worked very closely with the stem cell storage team to provide the hospital with all the information required to arrange a possible stem cell reinfusion.
The Transatlantic Journey
In April 2014, Paige’s umbilical cord blood stem cells were transferred to Duke University in North Carolina to use in a stem cell transplant. This involved the use of her own stored cells in an experimental treatment designed to address the tissue damage in her brain.
“Just two months after the reinfusion took place, Paige was crawling, pulling herself up onto furniture and standing while holding my hand, which we never thought she would ever be able to do,” says Carla. “It’s difficult to know whether her progress was due to natural development or due to the reinfusion but there is no doubt about the advances she has made. She just seems to be improving all the time.”
Carla and Kyle agree that their decision to collect and store Paige’s stem cells when she was born was the best investment they have ever made.
“Obviously the cost is a big factor but when you look at the bigger picture, collecting and storing your child’s stem cells could save their life – and that is something you can’t put a price on. Life is precious and you never know what lies around the corner.”
Expanding the Horizon: The Next Generation of Treatments
The stories of Sasha, Ahmed, and Paige represent only a small fraction of what modern medicine is achieving. As we move further into 2026, the potential applications for stem cell therapies are expanding into areas that were once thought untreatable. Through rigorous stem cell research, we are learning how to manipulate different types of cells to target specific diseases.
Autoimmune and Chronic Diseases
Current research is heavily focused on using mesenchymal stem cells (MSCs) to treat autoimmune diseases like rheumatoid arthritis and Crohn’s disease. MSCs are unique because they have immunomodulatory properties; they can “calm down” an overactive immune system, providing a path toward long-term remission without the heavy side effects of traditional immunosuppressants.
Cardiovascular and Heart Disease
Heart failure and the aftermath of a heart attack remain leading causes of death globally. However, recent studies in regenerative medicine are investigating the use of stem cells to repair heart muscle. By injecting new cells into damaged adipose tissue or directly into the heart muscle, researchers hope to stimulate the growth of new blood vessels and muscle cells, restoring function to the heart.
Neurodegenerative Diseases
Conditions such as Parkinson’s disease and multiple sclerosis (MS) are at the center of ongoing clinical trials. Using transcription factors to create iPS cells (induced pluripotent stem cells), scientists are working on creating new nerve cells to replace those lost to disease. This offers a glimmer of hope for patients suffering from spinal cord injuries or neurodegenerative decline, aiming for significant pain relief and restored mobility.
Macular Degeneration and Vision
Stem cell-based therapies are also making waves in ophthalmology. For those suffering from macular degeneration, clinical applications are being tested where specific cell types are grown ex vivo and transplanted into the eye to replace damaged retinal cells, potentially restoring sight to thousands of patients.
A Precaution Beyond Price
For the parents of Sasha, Paige and Ahmed, storing their babies’ stem cells at birth proved to be a life-changing step. For Mohammed Ahmed and his wife, there was already a pressing need, but for Tania and Richard Browne as well as Kyle and Carla Poppleton, the decision was made as a precaution – and a very wise one, as it turned out.
Banking your newborn’s umbilical cord blood is a small, simple step that could reap invaluable benefits later in life. It is an investment that more and more people are making to give them unprecedented peace of mind over the health of their child. Indeed, it’s not too much of a stretch to imagine a time when everybody on Earth has a supply of their own stem cells banked as part of their own personal healthcare programme, but for parents preparing for the birth of their next child, the opportunity to take advantage of this breakthrough technology is here right now.
FAQs: Accessing and Understanding Stem Cell Treatment
How do I access stem cell treatments for my family?
Accessing stem cell treatment usually begins with having your own banked sample. Here at Smart Cells, we’re a private umbilical cord blood bank, which means that we collect cord blood at birth, process the sample for your to collect the stem cells, and store these stem cells for you in our secure facility. If a family member is diagnosed with a treatable medical condition, your first step is to contact your stem cell bank (such as Smart Cells). We work directly with your transplant physician to arrange the release and transport of the sample to the treating facility. If you are looking for experimental treatments or clinical trials, your healthcare provider can help you find registered studies at institutions like Duke University or through the NHS clinical trials registry.
What if I haven’t stored my baby’s stem cells privately?
If you did not store cord blood at birth, your family can still access treatment through public bone marrow and cord blood registries if a medical need arises. While private storage provides an exclusive, 100% genetic match for your child, public registries like Anthony Nolan or the NHS Cord Blood Bank work to find compatible donors from a global pool. Additionally, advancements in stem cell research mean that adult stem cells can often be harvested from bone marrow or peripheral blood later in life for specific medical procedures. As mentioned, it can be harder to find a compatible match, especially if you are from an ethnic minority group where the chance of finding a matching donor can be as low as 29% compared to the chance of finding a match for a person with a white caucasian background which is 79%. This is why private cord blood banking can be such an important factor for many families.
Who are good candidates for stem cell therapy?
Good candidates for stem cell therapy are typically individuals with conditions that have been proven to respond to stem cell-based therapies, such as blood cancers, bone marrow failures, or certain genetic disorders. For emerging treatments like those for cerebral palsy or autism, candidacy is often determined by the specific requirements of a clinical trial, including the age of the patient and the availability of their own (autologous) cord blood.
Can stem cells from one child be used for another family member?
Yes. Cord blood stem cells can be used for treatment in both the patient’s own body as well as in family members who are a match. This opens up the potential of stem cells in treatment for families by an extraordinary amount. Stem cells from umbilical cord blood are often used for siblings, as there is a high probability of a genetic match. In some cases, they can even be used for parents or other relatives, though the chance of a successful match is lower. This is why many families choose to bank the cord blood of every child to ensure that the best possible match is always available.
Are these treatments considered a standard medical procedure?
It depends on the condition. For leukaemia, thalassemia, and over 80 other blood-related disorders, stem cell transplants are a standard, internationally recognized medical procedure. For conditions like cerebral palsy, heart disease, or diabetes, the use of stem cells is currently considered an experimental treatment and is primarily accessed through clinical trials.
What is the role of stem cell technology in cancer treatment?
Stem cell technology is a cornerstone of modern cancer treatment, particularly for blood-related cancers. After high-dose chemotherapy or radiation has destroyed a patient’s cancerous cells (and their healthy bone marrow), a stem cell transplant is used to repopulate the body with healthy, non-cancerous blood cells, effectively giving the patient a new immune system.
Understanding the Sources: Cord Blood vs. Other Stem Cells
While the potential of stem cells is vast, not all stem cells are created equal. In modern medicine, healthcare providers generally categorise stem cells based on where they are sourced and what specific cell types they can become.
- Cord Blood Stem Cells (Haematopoietic): These are found in the umbilical cord at birth. They are powerful immature cells that haven’t been exposed to environmental toxins or aging. They are primarily used to rebuild the immune system and treat blood cancers and genetic disorders.
- Cord Tissue Stem Cells (Mesenchymal): Also collected at birth, these cells are the masters of tissue repair. Research suggests they are good candidates for treating various tissues, including bone, cartilage, and muscle.
- Adult Stem Cells (Bone Marrow & Peripheral Blood): These are harvested later in life. While they are an effective treatment for many, the harvesting process can be invasive, and the cells may not be as potent or as “flexible” as those collected at birth.
By storing cord blood and tissue especially, which are the types of stem cells we specialise in at Smart Cells, you are capturing the most pristine, undifferentiated cells possible, providing a powerful tool for regenerative medicine that can’t be replicated later in life.
A Legacy of Health
The human body has an incredible capacity for healing, and stem cell biology is the key to unlocking that potential. Whether it is treating a heart attack, repairing a spinal cord injury, or overcoming a blood cancer, the use of stem cells represents the most powerful tool in our medical arsenal.
Navigating your pregnancy and preparing for the birth of your child is a time of great hope. By choosing to bank your baby’s cord blood, you are not just storing cells, you are storing potential. You are ensuring that if your family ever faces a medical challenge, you have the most advanced treatment options already waiting in the bank.
About the author: Shamshad Ahmed, CEO and Founder of Smart Cells International.
Shamshad Ahmed is CEO and Founder of Smart Cells International Ltd. Opening in 2000, Smart Cells became the UK’s first private cord blood company – its goal to give parents more access to potentially life-saving treatment for their families. It is one of the UK’s largest private banks, operating across the globe and storing over 50,000 cord blood samples from people in over 70 countries.
Rate this article: